PREVALENCE AND ASSOCIATED FACTORS IN THE DECLINE OF RENAL FUNCTION AMONG OUTPATIENTS ATTENDING A COMMUNITY HOSPITAL, CENTRAL THAILAND
DOI:
https://doi.org/10.55374/jseamed.v5i2.90Keywords:
Decline of renal function, Community hospital, NSAIDs, Pulse pressure, Prevalence, ThailandAbstract
Introduction: Chronic kidney disease (CKD) is recognized as global public health issue especially affecting developing countries including Thailand. The epidemiologic data in the decline of renal function and the risk factors among Thai patients especially in community hospital settings were limited.
Methods: A cross-sectional study was conducted to identify the prevalence and associated risk factors in the decline of renal function among outpatients in Thaluang Community Hospital, Lop Buri Province, central Thailand, between November 1, 2018 and October 31, 2019. The decline in renal function was defined by glomerular filtration rate (GFR) <60 mL/min/1.73m2. Multivariate logistic regression analysis was performed to obtain the adjusted odds ratios (AOR) and 95% confidence interval (CI) of the factors related to the decline of renal function.
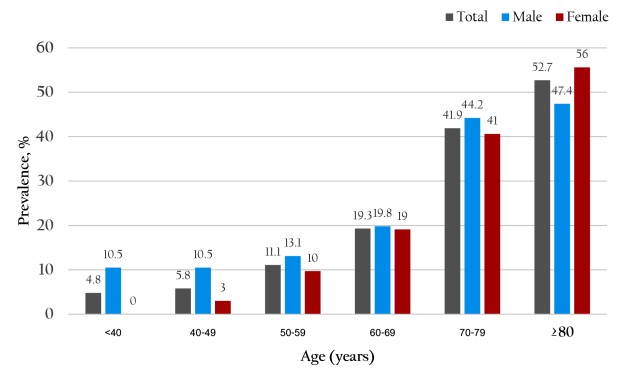
Results: A total of 874 outpatients participated in the study. The overall prevalence in the decline of renal function (eGFR <60 mL/min/1.73m2) was 20.3% (95% CI; 17.5%-22.9%). Among male participants, the prevalence in the decline of renal function was 21.1% (95%CI; 16.7%-25.5%) while it totaled 19.7% (95%CI; 16.3%-23.1%) among females. The independent associated factors in the decline of renal function included greater age (AOR 1.07; 95% CI=1.05-1.09), history of NSAIDs used (AOR 2.97; 95% CI=1.85-4.79) and elevated pulse pressure (PP) >75th percentile (AOR 1.64; 95% CI=1.07-2.53)
Conclusion: We reported the prevalence in the decline of renal function among outpatients in a Thai community hospital which was comparable with the national level. Advanced age, history of NSAIDs used and PP were related to reduced kidney function. Therefore, effective health interventions should be conducted especially, appropriate NSAIDs used among outpatients.
Downloads
Metrics
References
Abraham G, Varughese S, Thandavan T, Iyengar A, Fernando E, Naqvi SA, et al. Chronic kidney disease hotspots in developing countries in South Asia. Clin Kidney J 2016; 9: 135–41. DOI: https://doi.org/10.1093/ckj/sfv109
Awuah KT, Finkelstein SH, Finkelstein FO. Quality of life of chronic kidney disease patients in developing countries. Kidney Int Suppl 2013; 3: 227–9. DOI: https://doi.org/10.1038/kisup.2013.20
Ingsathit A, Thakkinstian A, Chaiprasert A, Sangthawan P, Gojaseni P, Kiattisunthorn K, et al. Prevalence and risk factors of chronic kidney disease in the Thai adult population: Thai SEEK study. Nephrol Dial Transplant 2010; 25: 1567–75. DOI: https://doi.org/10.1093/ndt/gfp669
Eriksen BO, Ingebretsen OC. The progression of chronic kidney disease: A 10-year populationbased study of the effects of gender and age. Kidney Int 2006; 69: 375–82. DOI: https://doi.org/10.1038/sj.ki.5000058
Rifkin DE, Shlipak MG, Katz R, Fried LF, Siscovick D, Chonchol M, et al. Rapid kidney function decline and mortality risk in older adults. Arch Inter Med 2008; 168: 2212–8. DOI: https://doi.org/10.1001/archinte.168.20.2212
Kazancioğlu R. Risk factors for chronic kidney disease: an update. Kidney Int Suppl 2013; 3: 368–71. DOI: https://doi.org/10.1038/kisup.2013.79
Duan J, Wang C, Liu D, Qiao Y, Pan S, Jiang D, et al. Prevalence and risk factors of chronic kidney disease and diabetic kidney disease in Chinese rural residents: a cross-sectional survey. Sci Rep 2019; 9: 10408. DOI: https://doi.org/10.1038/s41598-019-46857-7
Tótoli C, Carvalho AB, Ammirati AL, Draibe SA, Canziani MEF. Associated factors related to chronic kidney disease progression in elderly patients. PloS One 2019; 14: e0219956 DOI: https://doi.org/10.1371/journal.pone.0219956
ICD-10 World Health Organization: international statistical classification of diseases and related health problems: 10th reprint in 2015. http://www.who.int/classifications
Levey AS, Stevens LA, Schmid CH, Zhang YL, Castro 3rd AF, Feldman HI, et al. A new equation to estimate glomerular filtration rate. Ann Intern Med 2009; 150: 604–12. DOI: https://doi.org/10.7326/0003-4819-150-9-200905050-00006
Levey AS, de Jong PE, Coresh J, Nahas ME l., Astor BC, Matsushita K, et al. The definition, classification, and prognosis of chronic kidney disease: a KDIGO Controversies Conference report. Kidney Int 2011; 80: 17–28. DOI: https://doi.org/10.1038/ki.2010.483
Hirst JA, Hill N, O’ Ordóñez CA, Lasserson D, McManus RJ,Ogburn E. et al. Prevalence of chronic kidney disease in the community using data from OxRen: A UK populationbased cohort study. Br J Gen Pract 2020; 70: e285-93. DOI: https://doi.org/10.3399/bjgp20X708245
Chukwuonye II, Ohagwu KA, Adelowo OO, Chuku A, Obi EC, Onwuchekwa U, et al. Prevalence and Predictors of Chronic Kidney Disease in a Semiurban Community in Lagos. Inter J Nephrol 2019; 2019: 1625837 DOI: https://doi.org/10.1155/2019/1625837
Jayasekara JMKB, Dissanayake DM, Sivakanesan R, Ranasinghe A, Karunarathna RH, Priyantha Kumara GWG. Epidemiology of chronic kidney disease, with special emphasis on chronic kidney disease of uncertain etiology, in the North Central Region of Sri Lanka. J Epi 2015; 25: 275-80. DOI: https://doi.org/10.2188/jea.JE20140074
Delanaye P, Jager KJ, Bökenkamp A, Christensson A, Dubourg L, Eriksen BO, et al. CKD: A call for an age-adapted definition. J Am Soc Nephrol 2019; 30: 1785-1850. DOI: https://doi.org/10.1681/ASN.2019030238
Pan Y, Zhang L, Wang F, Li X, Wang H. Status of non-steroidal anti-inflammatory drugs use and its association with chronic kidney disease: A cross-sectional survey in China. Nephrol 2014; 19: 655-60. DOI: https://doi.org/10.1111/nep.12318
Gooch K, Culleton BF, Manns BJ, Zhang J, Alfonso H, Tonelli M, et al. NSAID Use and Progression of Chronic Kidney Disease. Am J Med 2007; 120: 280.e1-7. DOI: https://doi.org/10.1016/j.amjmed.2006.02.015
Lucas GNC, Leitão ACC, Alencar RL, Xavier RMF, Daher EDF, Silva Junior GB da. Pathophysiological aspects of nephropathy caused by non-steroidal anti-inflammatory drugs. J Bras Nefrol 2019: 41: 124–30. DOI: https://doi.org/10.1590/2175-8239-jbn-2018-0107
Levey AS, Coresh J. Chronic kidney disease. Lancet 2012; 379: 165–80. DOI: https://doi.org/10.1016/S0140-6736(11)60178-5
Atta MG, Whelton A. Acute renal papillary necrosis induced by ibuprofen. Am J Ther 1997; 4 : 55–60. DOI: https://doi.org/10.1097/00045391-199701000-00011
Luanghirun P, Tanaboriboon P, Mahissarakul P, Lertvivatpong N. Prevalence and associated factors of regular nonsteroidal anti-inflammatory drugs used in a rural community, Thailand. Glob J Health Sci 2017; 9: 58. DOI: https://doi.org/10.5539/gjhs.v9n9p58
Raina R, Polaconda S, Nair N, Chakraborty R, Sethi S, Krishnappa V, et al. Association of pulse pressure, pulse pressure index, and ambulatory arterial stiffness index with kidney function in a cross-sectional pediatric chronic kidney disease cohort from the CKiD study. J Clin Hypertens 2020; 22: 1059–69. DOI: https://doi.org/10.1111/jch.13905
Townsend RR, Chirinos JA, Parsa A, Weir MA, Sozio SM, Lash JP, et al. Central pulse pressure in chronic kidney disease: A chronic renal insufficiency cohort ancillary study. Hypertension 2010; 56: 518–24. DOI: https://doi.org/10.1161/HYPERTENSIONAHA.110.153924
Euswas N, Phonnopparat N, Morasert K, Thakhampaeng P, Kaewsanit A, Mungthin M, et al. National trends in the prevalence of diabetic retinopathy among Thai patients with type 2 diabetes and its associated factors from 2014 to 2018. PLoS One 2021; 16: e0245801. DOI: https://doi.org/10.1371/journal.pone.0245801
Steppan J, Barodka V, Berkowitz DE, Nyhan D. Vascular Stiffness and Increased Pulse Pressure in the Aging Cardiovascular System. Cardio Res Prac 2011; 2011: 263585. DOI: https://doi.org/10.4061/2011/263585
Avolio AP, Kuznetsova T, Heyndrickx GR, Kerkhof PLM, Li JK-J. Arterial Flow, Pulse Pressure and Pulse Wave Velocity in Men and Women at Various Ages. In: Kerkhof PLM, Miller VM, editors. Sex-Specific Analysis of Cardiovascular Function Cham: Springer International Publishing; 2018. pp. 153–68. DOI: https://doi.org/10.1007/978-3-319-77932-4_10
Xiao W, Wen Y, Ye P, Wang F, Cao R, Bai Y, et al. Noninvasive central pulse pressure is an independent determinant of renal function. J Clin Hypertens 2020; 22: 234–42. DOI: https://doi.org/10.1111/jch.13792
Downloads
Published
How to Cite
Issue
Section
License
The Journal of Southeast Asian Medical Research will hold the copyright to all published articles. The publisher's production department handles copyright forms once a manuscript is accepted and scheduled for publication.







