DURAL REPAIR: EFFICACY ASSESSMENT OF DIFFERENT TECHNIQUES, A CADAVERIC STUDY COMPARING THE NAKED EYE AND SURGICAL LOUPES
DOI:
https://doi.org/10.55374/jseamed.v5i1.81Keywords:
Dural tear, Dural repair, CSF leakageAbstract
Background: Watertight dural repair is crucial to achieve successful dural tear sutures. Microscopic or surgical loupes are recommended to use to magnify and assist repairing the dura. However, many spine surgeons repair dural tears under the naked eye. The efficacy of repairing dural tears by the naked eye compared with microscopic or surgical loupes has never been studied.
Objective: This study aimed to compare the efficacy of dural repairing techniques using the naked eye or surgical loupes.
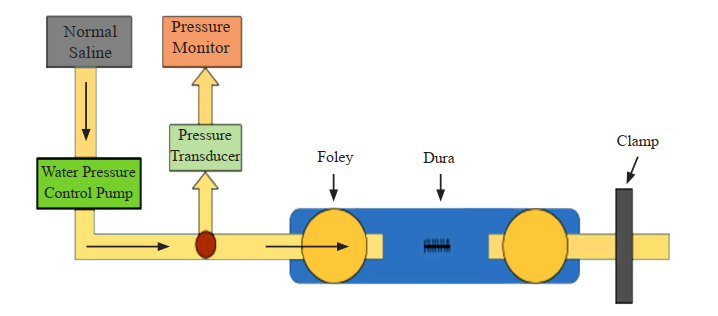
Methods: A cadaveric experimental study was conducted. Four fresh human cadaveric specimens were used to harvest the spinal cord. Dural tear and CSF leakage were simulated with a water pressure control system (Arthrex AR-6475 arthroscopic pump). We compared surgical repair using the naked eye and surgical loupes. Surgical closure was achieved using Prolene 6-0 and Durepair®. A total of 32 experimental dural tears were subdivided to four groups. The 4 groups were Prolene6-0 with the naked eye (n=8), Prolene 6-0 with surgical loupe (n = 8), Durepair® with the naked eye (n=8) and Durepair® with surgical loupe (n=8). The total time used for sutures and postsuture CSF water leakage pressure were recorded and compared among the subgroups.
Results: Our results showed that surgical loupe assisted dural closure and sutures were significantly faster than the naked eye in both Prolene 6-0 (surgical loupe = 4.87±0.19 min, naked eye = 7.18±0.36 min, p <0.001) and Durepair® groups (surgical loupe = 9.84±0.21 min naked eye = 13.27±0.42 min, p <0.001). CSF Leakage pressure in the surgical loupe groups were higher than in the naked eye groups in both Prolene 6-0 (surgical loupe = 100.00±5.35 mmHg, naked eye = 96.88±7.99 mmHg, p = 0.373) and Durepair® (surgical loupe = 96.88±4.58 mmHg, naked eye = 95.63±4.17 mmHg, p = 0.577) but without significant difference. Prolene 6-0 was significantly faster to use for sutures than Durepair® in both sutures by the naked eye and surgical loupe assisted (p <0.001). Prolene 6-0 showed a higher leakage pressure than Durepair® in both the naked eye and surgical loupe assisted sutures but without significant difference (naked eye, p = 0.701, surgical loupe, p = 0.230)
CONCLUSION: Repairing a dural tear without using surgical loupes consumed more time and did not achieve similar maximum leak pressure compared with using surgical loupes. However, no statistically significant difference was observed in terms of CSF leakage pressure. Durepair® consumed more time than Prolene 6-0 while leakage pressure was similar. We recommended the use of surgical loupes when performing dural repair. Durepair® is suitable to repair larger dural defects that cannot be closed using a simple suture technique.
Downloads
Metrics
References
Hannallah D, Lee J, Khan M, Donaldson WF, Kang JD. Cerebrospinal fluid leaks following cervical spine surgery. J Bone Joint Surg Am 2008; 90A: 1101-5. DOI: https://doi.org/10.2106/JBJS.F.01114
Saxler G, Kramer J, Barden B, Kurt A, Pförtner J, Bernsmann K The long-term clinical sequelae of incidental durotomy in lumbar disc surgery. Spine 2005; 30: 2298-302. DOI: https://doi.org/10.1097/01.brs.0000182131.44670.f7
Jones AA, Stambough JL, Balderston RA, Rothman RH, Booth Jr RE. Long-term results of lumbar spine surgery complicated by unintended incidental durotomy. Spine 1989; 14: 443–6. DOI: https://doi.org/10.1097/00007632-198904000-00021
Cammisa FP Jr, Girardi FP, Sangani PK, Parvataneni HK, Cadag S, Sandhu HS. Incidental durotomy in spine surgery. Spine 2000; 25: 2663-7. DOI: https://doi.org/10.1097/00007632-200010150-00019
Wang JC, Bohlman HH, Riew KD. Dural tears secondary to operations on the lumbar spine. Management and results after a two year- minimum follow-up of eighty-eight patients. J Bone Joint Surg Am 1998; 80: 1728-32. DOI: https://doi.org/10.2106/00004623-199812000-00002
Goodkin R, Laska LL. Unintended ‘‘incidental’’ durotomy during surgery of the lumbar spine: medicolegal implications. Surg Neurol 1995; 43: 4-12. DOI: https://doi.org/10.1016/0090-3019(95)80031-B
Kitchel SH, Eismont FJ, Green BA. Closed subarachnoid drainage for management of cerebrospinal fluid leakage after an operation on the spine. J Bone Joint Surg Am 1989; 71A: 984-7. DOI: https://doi.org/10.2106/00004623-198971070-00004
Eismont FJ, Wiesel SW, Rothman RH. Treatment of dural tears associated with spinal surgery. J Bone Joint Surg Am 1981; 63A: 1132-6. DOI: https://doi.org/10.2106/00004623-198163070-00010
Chen YX, Chen LE, Seaber AV, Urbaniak JR. Comparison of continuous and interrupted suture techniques in microvascular anastomosis. J Hand Surg Am 2001; 26: 530-9. DOI: https://doi.org/10.1053/jhsu.2001.22933
Cain JE Jr, Dryer RF, Barton BR. Evaluation of dural closure techniques. Suture methods, fibrin adhesive sealant, and cyanoacrylate polymer. Spine 1988; 13: 720-5. DOI: https://doi.org/10.1097/00007632-198807000-00002
Erica E. Dafford, Paul A. Anderson. Comparison of dural repair techniques. Spine 2015; 15: 1099-105. DOI: https://doi.org/10.1016/j.spinee.2013.06.044
Luca Papavero, Nils Engler, Ralph Kothe. Incidental durotomy in spine surgery: first aid in ten steps. Eur Spine J 2015; 24: 2077-84. DOI: https://doi.org/10.1007/s00586-015-3837-x
Lee S, Frank DH, Chou SY. Historical review of small and microvascular vessel surgery. Ann Plast Surg 1983; 11: 53-62. DOI: https://doi.org/10.1097/00000637-198307000-00008
Davidson BJ, Guardiani E, Wang A. Adopting the operating microscope in thyroid surgery: safety, efficiency, and ergonomics. Head Neck 2010; 32154-59. DOI: https://doi.org/10.1002/hed.21157
Serletti JM, Deuber MA, Guidera PM, Reading G, Herrera HR, Reale VF, et al. Comparison of the operating microscope and loupes for free microvascular tissue transfer. Plast Reconstr Surg 1995; 95: 270-76. DOI: https://doi.org/10.1097/00006534-199502000-00006
Pieptu D, Luchian S. Loupes-only microsurgery. Microsurgery 2003; 23: 181-88. DOI: https://doi.org/10.1002/micr.10126
Shenaq SM, Klebuc MJ, Vargo D. Free-tissue transfer with the aid of loupe magnification: experience with 251 procedures. Plast Reconstr Surg 1995; 95: 261-69.
Andrades P, Benitez S, Danilla S, Erazo C, Hasbun A, Fix J. Vascular diameter determining the magnification for a microvascular anastomosis. Reconstr Microsurg 2008; 24: 174-81.
Andrades P, Benitez S, Danilla S, Erazo C, Hasbun A, Fix J. Vascular diameter determining the magnification for a microvascular anastomosis. Reconstr Microsurg 2008; 24: 174-81. DOI: https://doi.org/10.1055/s-2008-1076084
Shenaq SM, Klebuc MJ, Vargo D. Free-tissue transfer with the aid of loupe magnification: experience with 251 procedures. Plast Reconstr Surg 1995; 95:261-69. DOI: https://doi.org/10.1097/00006534-199502000-00005
Ross DA, Ariyan S, Restifo R, Sasaki CT. Use of the operating microscope and loupes for head and neck free microvascular tissue transfer. Arch Otolaryngol Head Neck Surg 2003; 129: 189 -93. DOI: https://doi.org/10.1001/archotol.129.2.189
Downloads
Published
How to Cite
Issue
Section
License
The Journal of Southeast Asian Medical Research will hold the copyright to all published articles. The publisher's production department handles copyright forms once a manuscript is accepted and scheduled for publication.







