RECOVERY OF HEMOGLOBIN LEVEL FOLLOWING TOTAL KNEE ARTHROPLASTY WITH PERIARTICULAR EPINEPHRINE INJECTION
DOI:
https://doi.org/10.55374/jseamed.v3i1.47Keywords:
Total knee arthroplasty, Periarticular epinephrine injection, Hemoglobin recovery, Randomized-controlled trialAbstract
Background: Anemia is one of the common complications occurring after total knee arthroplasty (TKA). A periarticular epinephrine injection could reduce intraoperative blood loss after TKA. However, the duration of hemoglobin recovery to preoperative level remains uncertain. The hypothesis was based on the concept that epinephrine affects vasoconstriction and reduces blood loss. This study was conducted to compare the duration of hemoglobin recovery to preoperative level between periarticular epinephrine injection and periarticular nonepinephrine injection groups and postoperative blood transfusion.
Methods: A total of 141 participants were randomized to receive a periarticular epinephrine and bupivacaine injection (epinephrine group) or periarticular bupivacaine injection (non-epinephrine group) among patients undergoing TKA. The solution consisted of 10 g of epinephrine 1 ml and 20 ml of 0.25% bupivacaine. In another group, the solution consisted of 20 ml of 0.25% bupivacaine alone. All TKAs were managed under spinal anesthesia using a femoral nerve block. Preoperative and postoperative hemoglobin (Hb) and hematocrit (Hct) levels were assessed 1-day, 3-day and monthly until 6 months. Blood loss and the duration of Hb recovery to preoperative level were compared between the two groups.
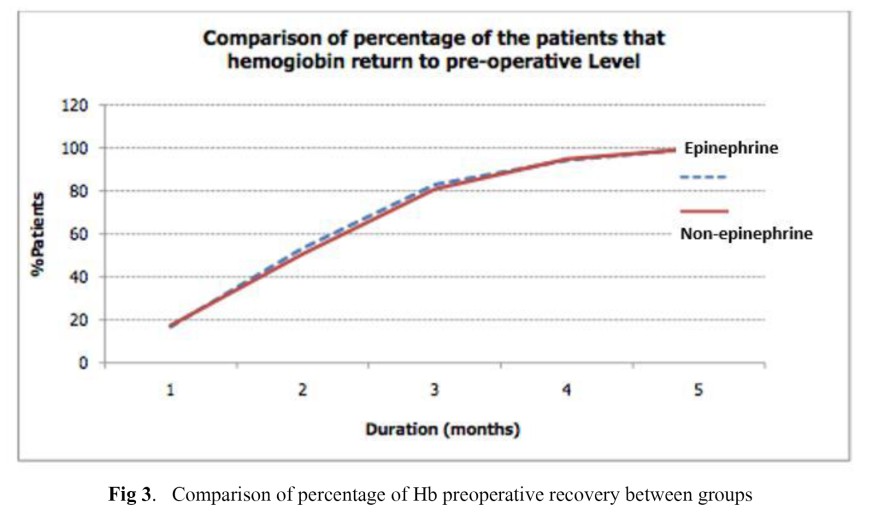
Results: The percentage of Hb loss was slightly higher in the epinephrine group than that in the nonepinephrine group but without significance (13.4 ± 6.6% vs. 13.01 ± 5.01%; p=0.703). The duration of Hb recovery to preoperative level was about the same in the epinephrine and nonepinephrine groups (2.52 ± 1.080 months vs. 2.56 ± 1.089 months; p=0.855). The calculated total blood loss in the epinephrine group was lower than that in the nonepinephrine group (570 ± 302 mL vs. 573 ± 228 mL; p=0.955). In this study, surgery was performed without blood transfusions.
Conclusion: The duration of Hb recovery to preoperative level was 2.5 months which was about the same in both groups. Epinephrine injection did not decrease total blood volume loss after TKA under spinal anesthesia.
Downloads
Metrics
References
Tsukada S, Wakui M, Hoshino A. Postoperative epidural analgesia compared with intraoperative periarticular injection for pain control following total knee arthroplasty under spinal anesthesia: a randomized controlled trial. J Bone Joint Surg Am 2014; 96: 1433-8. DOI: https://doi.org/10.2106/JBJS.M.01098
Jasper LL, Jones CA, Mollins J, Pohar SL, Beaupre LA. Risk factors for revision of total knee arthroplasty: a scoping review. BMC Musculoskelet Disord 2016; 17: 182. DOI: https://doi.org/10.1186/s12891-016-1025-8
Anderson LA, Engel GM, Bruckner JD, Stoddard GJ, Peters CL. Reduced blood loss after total knee arthroplasty with local injection of bupivacaine and epinephrine. J Knee Surg 2009; 22: 130-6. DOI: https://doi.org/10.1055/s-0030-1247737
Kurosaka K, Tsukada S, Seino D, Morooka T, Nakayama H, Yoshiya S. Local infiltration analgesia versus continuous femoral nerve block in pain relief after total knee arthroplasty: A randomized controlled trial. J Arthroplasty 2016; 31: 913-7. DOI: https://doi.org/10.1016/j.arth.2015.10.030
Fan L, Yu X, Zan P, Liu J, Ji T, Li G. Comparison of local iInfiltration analgesia with femoral nerve block for total knee arthroplasty: A prospective, randomized clinical trial. J Arthroplasty 2016; 31: 1361-5. DOI: https://doi.org/10.1016/j.arth.2015.12.028
Nakagawa S, Arai Y, Inoue H, Kan H, Hino M, Ichimaru S, et al. Comparative effects of periarticular multimodal drug injection and single-shot femoral nerve block on pain following total knee arthroplasty and factors influencing their effectiveness. Knee Surg Relat Res 2016; 28: 233-8. DOI: https://doi.org/10.5792/ksrr.2016.28.3.233
Lombardi AV, Jr., Berend KR, Mallory TH, Dodds KL, Adams JB. Soft tissue and intra-articular injection of bupivacaine, epinephrine, and morphine has a beneficial effect after total knee arthroplasty. Clin Orthop Relat Res 2004: 125-30. DOI: https://doi.org/10.1097/01.blo.0000147701.24029.cc
Lacher DA, Barletta J, Hughes JP. Biological variation of hematology tests based on the 1999-2002 National Health and Nutrition Examination Survey. Natl Health Stat Report 2012: 1-10.
Zhou Q, Zhou Y, Wu H, Wu Y, Qian Q, Zhao H, et al. Changes of hemoglobin and hematocrit in elderly patients receiving lower joint arthroplasty without allogeneic blood transfusion. Chin Med J (Engl) 2015; 128: 75-8. DOI: https://doi.org/10.4103/0366-6999.147817
Erskine JG, Fraser C, Simpson R, Protheroe K, Walker ID. Blood loss with knee joint replacement. J R Coll Surg Edinb 1981; 26: 295-7.
Sehat KR, Evans RL, Newman JH. Hidden blood loss following hip and knee arthroplasty.Correct management of blood loss should take hidden loss into account. J Bone Joint Surg Br 2004; 86: 561-5. DOI: https://doi.org/10.1302/0301-620X.86B4.14508
Stucinskas J, Tarasevicius S, Cebatorius A, Robertsson O, Smailys A, Wingstrand H. Conventional drainage versus four hour clamping drainage after total knee arthroplasty in severe osteoarthritis: a prospective, randomised trial. Int Orthop 2009; 33: 1275-8. DOI: https://doi.org/10.1007/s00264-008-0662-4
Wang D, Xu J, Zeng WN, Zhou K, Xie TH, Chen Z, et al. Closed suction drainage is not associated with faster recovery after total knee arthroplasty: A prospective randomized controlled study of 80 patients. Orthop Surg 2016; 8: 226-33. DOI: https://doi.org/10.1111/os.12247
Chotanaphuti T, Wangwittayakul V, Khuangsirikul S, Foojareonyos T. The accuracy of component alignment in custom cutting blocks compared with conventional total knee arthroplasty instrumentation: prospective control trial. Knee 2014; 21: 185-8. DOI: https://doi.org/10.1016/j.knee.2013.08.003
Gibon E, Courpied JP, Hamadouche M. Total joint replacement and blood loss: what is the best equation? Int Orthop 2013; 37: 735-9. DOI: https://doi.org/10.1007/s00264-013-1801-0
Prasad N, Padmanabhan V, Mullaji A. Blood loss in total knee arthroplasty: an analysis of risk factors. Int Orthop 2007; 31: 39-44. DOI: https://doi.org/10.1007/s00264-006-0096-9
Gao F, Sun W, Guo W, Li Z., Wang W, Cheng L. Topical administration of tranexamic acid plus diluted-epinephrine in primary total knee arthroplasty: A randomized double-blinded controlled trial. J Arthro 2015; 30: 1354-8. DOI: https://doi.org/10.1016/j.arth.2015.03.003
Holt BT, Parks NL, Engh GA, Lawrence JM. Comparison of closed-suction drainage and no drainage after primary total knee arthroplasty. Orthopedics 1997; 20: 1121-4; discussion 4-5. DOI: https://doi.org/10.3928/0147-7447-19971201-05
Jenny JY, Boeri C, Lafare S. No drainage does not increase complication risk after total knee prosthesis implantation: a prospective, comparative, randomized study. Knee Surg Sports Traumatol Arthrosc 2001; 9: 299-301. DOI: https://doi.org/10.1007/s001670100220
Downloads
Published
How to Cite
Issue
Section
License
The Journal of Southeast Asian Medical Research will hold the copyright to all published articles. The publisher's production department handles copyright forms once a manuscript is accepted and scheduled for publication.







