ACTIVITY OF TRIAZOLES AND ECHINOCANDINS AGAINST CANDIDA BLOODSTREAM ISOLATES AT PHRAMONGKUTKLAO HOSPITAL, THAILAND
DOI:
https://doi.org/10.55374/jseamed.v5i2.96Keywords:
Triazoles, Echinocandins, Candida spp., bloodstream infectionAbstract
Background: Candidemia is a major cause of morbidity and mortality which can be treated using antifungal agents, triazoles and echinocandins.
Objectives: We aimed to determine Candida species and their sensitivities to triazoles (fluconazole, itraconazole, voriconazole, and posaconazole) and echinocandins (caspofungin, micafungin, and anidulafungin) among patients with candidiasis to guide future treatment of patients with candidemia or invasive candidiasis.
Methods: All firstly isolated Candida spp. from patients admitted at Phramongkutklao Hospital, Bangkok, Thailand from January 2012 to December 2013 were included in this study. The antifungal susceptibility testing of Candida spp. isolates was assessed based on micro-dilution method.
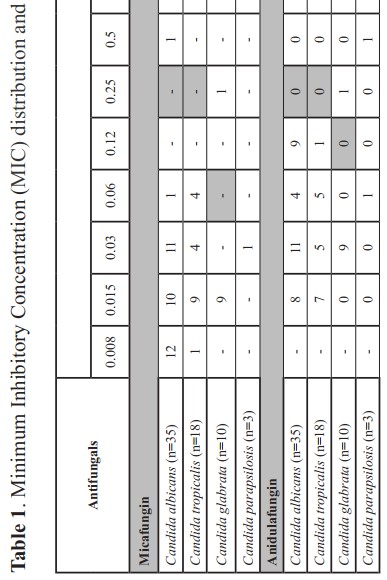
Results: During the 24-month study period, a total of 66 Candida isolates from 66 patients were identified. Of the 66 isolates, 35 (53%) were C. albicans, 18 (27.3%) were C. tropicalis, 10 (15.2%) were C. glabrata and 3 (4.5%) were C. parapsilosis. Fluconazole resistant Candida isolates were found in C. glabrata (100%), C. albicans (14.3%), C. tropicalis (22.2%) and C. parapsilosis (66.7%). Most Candida spp. isolates were mainly susceptible to echinocandins (>90%). Notably, 10%-20% of C. glabrata isolates showed resistance to echinocandins.
Conclusion: Fluconazole, an empirical therapy, has been cautiously used due to resistant non-albicans Candida species especially, C. glabrata, C. tropicalis and C. parapsilosis. However, the emerging echinocandins resistant C. glabrata isolates need to be closely monitored.
Downloads
Metrics
References
Enoch DA, Yang H, Aliyu SH, Micallef C. The changing epidemiology of invasive fungal infections. Methods Mol Biol 2017; 1508: 17-65. DOI: https://doi.org/10.1007/978-1-4939-6515-1_2
Koehler P, Stecher M, Cornely OA, Koehler D, Vehreschild M, Bohlius J, et al. Morbidity and mortality of candidaemia in Europe: an epidemiologic meta-analysis. Clin Microbiol Infect 2019; 10: 1200-12. DOI: https://doi.org/10.1016/j.cmi.2019.04.024
Guinea J. Global trends in the distribution of Candida species causing candidemia. Clin Microbiol Infect 2014; 20 (Suppl 6): 5-10. DOI: https://doi.org/10.1111/1469-0691.12539
Alexander BD, Johnson MD, Pfeiffer CD, Jimenez-Ortigosa C, Catania J, Booker R, et al. Increasing echinocandin resistance in Candida glabrata: clinical failure correlates with presence of FKS mutations and elevated minimum inhibitory concentrations. Clin Infect Dis 2013; 56: 1724-32. DOI: https://doi.org/10.1093/cid/cit136
Foongladda S, Sakulmaiwatana P, Petlum P, Vanprapar N. Candida species, genotypes and antifungal susceptibility of Candida isolates from blood samples of patients at the largest tertiary care hospital in Thailand during 1999-2002. J Med Assoc Thai 2004; 87: 92-9.
Tan TY, Hsu LY, Alejandria MM, Chaiwarith R, Chinniah T, Chayakulkeeree M, et al. Antifungal susceptibility of invasive Candida bloodstream isolates from the Asia-Pacific region. Med Mycol 2016; 54: 471-7. DOI: https://doi.org/10.1093/mmy/myv114
Jutiamornlerd N, Chusri S, Siripaitoon P. Epidemiology of candidemia in Songklanagarind Hospital. J Med Assoc Thai 2011; 94: 927-32.
Tan BH, Chakrabarti A, Li RY, Patel AK, Watcharananan SP, Liu Z, et al. Incidence and species distribution of candidaemia in Asia: a laboratory-based surveillance study. Clin Microbiol Infect 2015; 21: 946-53. DOI: https://doi.org/10.1016/j.cmi.2015.06.010
Chaiwarith R, Ounbang P, Khamwan C, Nuntachit N, Sirisanthana T, Supparatpinyo K. Epidemiology of adult candidemia at Chiang Mai University Hospital. Southeast Asian J Trop Med Public Health 2011; 42: 1505-14.
Pappas PG, Kauffman CA, Andes DR, Clancy CJ, Marr KA, Ostrosky-Zeichner L, et al. Clinical practice guideline for the management of candidiasis: 2016 Update by the Infectious Diseases Society of America. Clin Infect Dis 2016; 62: e1-50. DOI: https://doi.org/10.1093/cid/civ933
Ngamchokwathana C, Chongtrakool P, Waesamaae A, Chayakulkeeree M. Risk factors and outcomes of non-albicans Candida bloodstream infection in patients with candidemia at Siriraj Hospital-Thailand’s largest national tertiary referral hospital. J Fungi (Basel) 2021; 7: 269. DOI: https://doi.org/10.3390/jof7040269
Fernandez-Ruiz M, Aguado JM, Almirante B, Lora-Pablos D, Padilla B, Puig-Asensio M, et al. Initial use of echinocandins does not negatively influence outcome in Candida parapsilosis bloodstream infection: a propensity score analysis. Clin Infect Dis 2014; 58: 1413-21. DOI: https://doi.org/10.1093/cid/ciu158
Downloads
Published
How to Cite
Issue
Section
License
The Journal of Southeast Asian Medical Research will hold the copyright to all published articles. The publisher's production department handles copyright forms once a manuscript is accepted and scheduled for publication.







