Prevalence and effect of flatfoot among army privates
DOI:
https://doi.org/10.55374/jseamed.v1i2.29Keywords:
Flatfoot deformity, Army Private, Plantar Foot Pressure, Functional OutcomeAbstract
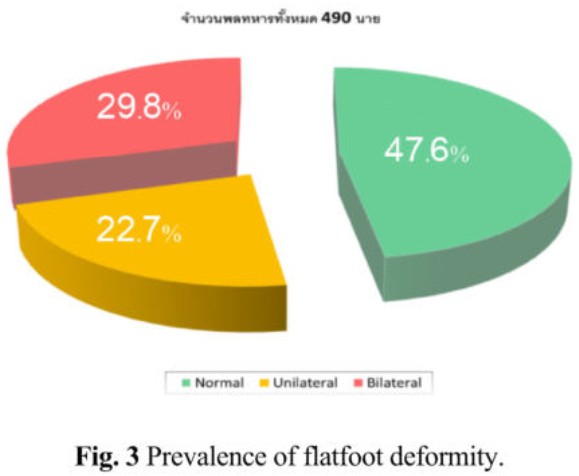
Background: Specific populations require strenuous activities such as soldiers, and flatfoot deformity can cause significant problems during training or operations. Prevalence of this deformity among Thai Army privates is limited and underestimated due to improper screening techniques. We would like to report the prevalence of flatfoot deformity using a new standardized device and compare performances of army privates between normal foot and flatfoot deformity Study design: The study employed a cross-sectional design Materials and Methods: A prospective study of 490 army privates in the King’s Guard, 2nd Cavalry Division, between June 2015 and November 2015 was conducted. Footprints were collected from all participant using a Harris Mat imprinter and the shape of their feet was recorded based on arch height. The Stahili index >0.77 (NY index) and arch height less than 6 mm were used as cut-off point values to diagnose flatfoot deformity. Additionally, military training performance (running 2 km) was evaluated using validated functional outcome (VAS-FA) and compared between normal arch and flatfoot deformity groups. Results: The prevalence of flatfoot deformity determined using footprints was 52.5% (233 participants: 111 of 233 participants were unilateral (47.6%) and 146 of 233 participants (52.3%) were bilateral flatfeet). The physical training revealed significant differences when compared between bilateral flatfeet and normal arch groups (p= 0.038) and bilateral flatfeet unilateral flatfoot groups (p= 0.009) BMI, VAS score and flatfoot deformity significantly affected the performances of their training (p= 0.03, 0.02, and 0.03 for BMI, VAS score and flatfoot deformity, respectively.) Conclusion: The prevalence of flatfeet deformity among army privates from this study was higher than relates studies. Bilateral flatfeet deformity had a significant effect on physical training. Although many factors affect training performance, BMI, VAS score and flatfoot deformity significantly affected the military training program.
Downloads
Metrics
References
Lee MS, Vanore JV, Thmas JL, Catanzariti AR, Kogler G, Kravitz SR et al. Diagnosis and treatment of adult flatfoot. J Foot Ankle Surg 2005; 44: 78-113 DOI: https://doi.org/10.1053/j.jfas.2004.12.001
Vulcano E, Deland JT, Elis SJ. Approach and treatment of the adult acquired flatfoot deformity. Curr Rev Musculoskelet Med 2013; 6: 294-303 DOI: https://doi.org/10.1007/s12178-013-9173-z
Ferciot CF. The etiology of developmental flatfoot. Clin Orthop Relat Res 1972; 85: 7-10 DOI: https://doi.org/10.1097/00003086-197206000-00003
Levy JC, Mizel MS, Wilson LS, Fox W, McHale K, Taylor DC et al. Incidence of foot and ankle injuries in West Point cadets with pes planus compared to the general cadet population. Foot Ankle Int 2006; 27: 1060-4 DOI: https://doi.org/10.1177/107110070602701211
Harris RI, Beath T. Hypermobile flat-foot with short tendo achillis. J Bone Joint Surg Am 1948; 30A: 116-140 DOI: https://doi.org/10.2106/00004623-194830010-00013
Abdel-Fattah MM, Hassanin MM, Felembane FA, Nassaane MT. Flat foot among Saudi Arabian army recruits: prevalence and risk factors. East Mediyerr Health J 2006; 12: 211-7
Angthong C. Validity and reliability of Thai version of the foot and Ankle Outcome Score in patients with arthritis of the foot and ankle. Foot Ankle Surg 2016; 22: 224-8 DOI: https://doi.org/10.1016/j.fas.2015.09.006
Plumarom Y, Imjaijitt W, Chaiphrom N. Comparison between Staheli index on Harris mat footprint and Talar-first metatarsal angle for the diagnosis of flatfeet. J Med Assoc Thai 2014; 97 Suppl 2: S131-5
Staheli LT, Chew DE, Corbett M. The longitudinal arch. A survey of eight hundred and eight-two feet in normal children and adults. J Bone Joint Surg Am 1987; 69: 426-8 DOI: https://doi.org/10.2106/00004623-198769030-00014
A D. Pied plat valgus statique. In: Encyclopedia medico-chirurgicale appareil locomoteur. 1974: Paris, France, Editions Techniques.
Coughlin MJ, Kaz A. Correlation of Harris mats, physical exam, pictures, and radiographic measurements in adult flatfoot deformity. Foot Ankle Int 2009; 30: 604-12 DOI: https://doi.org/10.3113/FAI.2009.0604
Smyth NA, Aiyer AA, Kaplan JR, Carmody CA, Kadakia AR. Adult-acquired flatfoot deformity. Eur J Orthop Surg Traumatol 2017; 27: 433-9 DOI: https://doi.org/10.1007/s00590-017-1945-5
Downloads
Published
How to Cite
Issue
Section
License
The Journal of Southeast Asian Medical Research will hold the copyright to all published articles. The publisher's production department handles copyright forms once a manuscript is accepted and scheduled for publication.







