COMPARISON OF ANALGESIC EFFICACY BETWEEN ULTRASOUND-GUIDED ILIOHYPOGASTRIC/ILIOINGUINAL NERVE BLOCK AND WOUND INFILTRATION AMONG PATIENTS UNDERGOING GYNECOLOGIC SURGERY: A RANDOMIZED CONTROLLED TRIAL
DOI:
https://doi.org/10.55374/jseamed.v7.140Keywords:
Iliohypogastric/ilioinguinal nerve block, Gynecologic surgery, Local anesthetic, Postoperative painAbstract
Background: Postoperative pain control is essential after surgery to ensure early mobilization, decrease the length of hospital stay and provide patient comfort. Local anesthetic (LA) wound infiltration has been used to reduce postoperative pain. In addition, the bilateral iliohypogastric/ilioinguinal nerve block (IINB) has been used to control pain in abdominal surgery but not in gynecologic or pelvic surgery.
Objectives: This study aimed to evaluate the efficacy of ultrasound-guided iliohypogastric/ ilioinguinal nerve block compared with local anesthetic wound infiltration on postoperative pain control among patients undergoing gynecologic surgery through a Pfannenstiel incision.
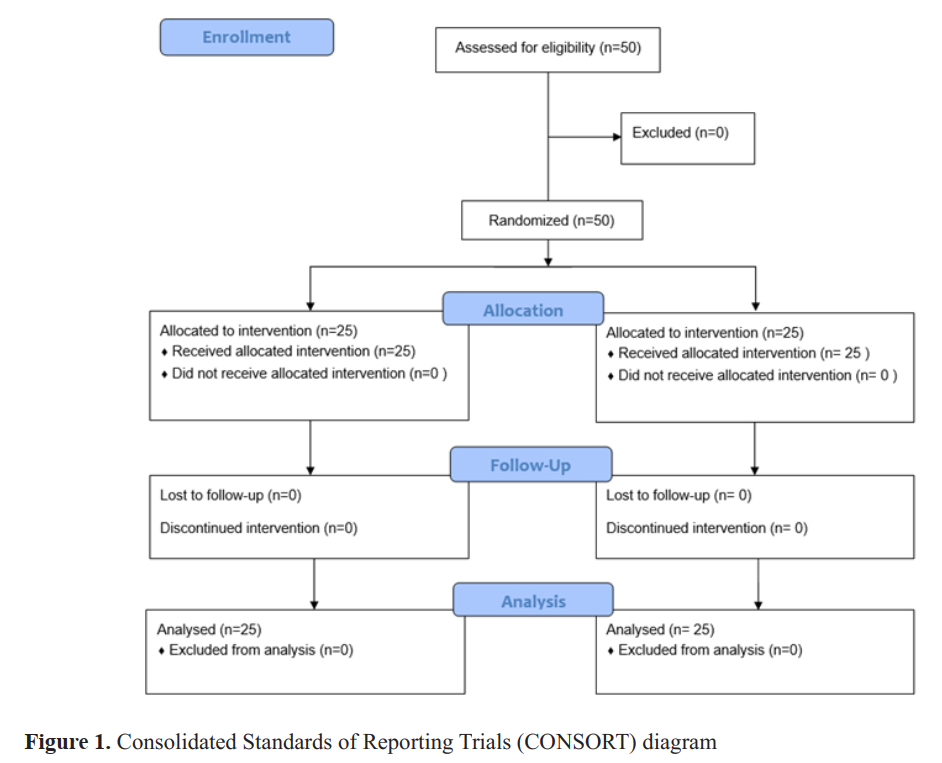
Methods: In this prospective, double-blinded, randomized controlled trial, 50 patients were allocated to either an IINB group (N=25) or LA group (N=25). In both groups, postoperative IV patient-control analgesia (PCA) was planned 24 hours, postoperatively. The primary outcomes were differences in pain score using a numerical rating scale (NRS) and morphine consumption between both groups immediately following 2, 4, 8, 12 and 24 hours, postoperatively.
Results: The postoperative pain scores were significantly lower in the IINB group than in the LA group at all time points, with p <0.05. Total morphine consumption for 2-24 hours postoperative was significantly lower in the IINB group than in the LA group with p <0.001.
Conclusion: Compared with LA wound infiltration, this study demonstrated that IINB provided better pain control and reduced the consumption of morphine in the first 24 hours among patients undergoing gynecologic surgery through a Pfannenstiel incision.
Downloads
Metrics
References
Bamigboye AA, Hofmeyr GJ. For postoperative pain relief, local anaesthetic wound infiltration and abdominal nerves block during caesarean section. Cochrane Database Syst Rev 2009: Cd006954. DOI: https://doi.org/10.1002/14651858.CD006954.pub2
Elia N, Lysakowski C, Tramèr MR. Does multimodal analgesia with acetaminophen, nonsteroidal anti-inflammatory drugs, or selective cyclooxygenase-2 inhibitors and patient-controlled analgesia morphine offer advantages over morphine alone? Meta-analyses of randomized trials. Anesthesiology 2005; 103: 1296-304. DOI: https://doi.org/10.1097/00000542-200512000-00025
White PF. The changing role of non-opioid analgesic techniques in the management of postoperative pain. Anesth Analg 2005; 101(5 Suppl): S5-s22. DOI: https://doi.org/10.1213/01.ANE.0000177099.28914.A7
Eichenberger U, Greher M, Kirchmair L, Curatolo M, Moriggl B. Ultrasound-guided blocks of the ilioinguinal and iliohypogastric nerve: accuracy of a selective new technique confirmed by anatomical dissection. Br J Anaesth 2006; 97: 238-43. DOI: https://doi.org/10.1093/bja/ael103
Bessmertnyj AE, Antipin EE, Uvarov DN, Sedyh SV, Nedashkovsky EV. Comparison of the effectiveness of ilioinguinal-iliohypogastric blockade and transversus abdominis plane block for analgesia after cesarean section. Anesteziol Reanimatol 2015; 60: 51-4.
Kelly MC, Beers HT, Huss BK, Gilliland HM. Bilateral ilioinguinal nerve blocks for analgesia after total abdominal hysterectomy. Anaesthesia 1996; 51: 406. DOI: https://doi.org/10.1111/j.1365-2044.1996.tb07768.x
Wang Y, Wu T, Terry MJ, Eldrige JS, Tong Q, Erwin PJ, et al. Improved perioperative analgesia with ultrasound-guided ilioinguinal/ iliohypogastric nerve or transversus abdominis plane block for open inguinal surgery: a systematic review and meta-analysis of randomized controlled trials. J Phys Ther Sci 2016; 28: 1055-60. DOI: https://doi.org/10.1589/jpts.28.1055
Elahwal L, Elrahwan S, Elbadry AA. Ilioinguinal and Iliohypogastric Nerve Block for Acute and Chronic Pain Relief After Caesarean Section: A Randomized Controlled Trial. Anesth Pain Med 2022; 12: e121837. DOI: https://doi.org/10.5812/aapm.121837
Saboo V, Biswas D, Naz A, Seal S, Ray R. Local Infiltration of Bupivacaine along the Incision Line following Cesarean Section reduces Postoperative Pain and Analgesia Requirement: A Double-blinded Randomized Controlled Study. J South Asian Feder Obs Gynae 2022; 14: 596-601. DOI: https://doi.org/10.5005/jp-journals-10006-2114
Sivapurapu V, Vasudevan A, Gupta S, Badhe AS. Comparison of analgesic efficacy of transversus abdominis plane block with direct infiltration of local anesthetic into surgical incision in lower abdominal gynecological surgeries. J Anaesthesiol Clin Pharmacol 2013;29:71-5. DOI: https://doi.org/10.4103/0970-9185.105807
Ng A, Swami A, Smith G, Davidson AC, Emembolu J. The analgesic effects of intraperitoneal and incisional bupivacaine with epinephrine after total abdominal hysterectomy. Anesth Analg 2002; 95: 158-62. DOI: https://doi.org/10.1097/00000539-200207000-00028
Tubbs RS, Rizk EB, Shoja M, Loukas M, Barbaro N, Spinner RJ. Nerves and Nerve Injuries: Vol 2: Pain, Treatment, Injury, Disease and Future Directions: Elsevier Science; 2015.
Gofeld M, Christakis M. Sonographically guided ilioinguinal nerve block. J Ultrasound Med 2006; 25: 1571-5 14. Okur O, Tekgul ZT, Erkan N. Comparison of efficacy of transversus abdominis plane block and iliohypogastric/ilioinguinal nerve block for postoperative pain management in patients undergoing inguinal herniorrhaphy with spinal anesthesia: a prospective randomized controlled open-label study. J Anesth 2017; 31: 678-85. DOI: https://doi.org/10.1007/s00540-017-2378-3
Yu N, Long X, Lujan-Hernandez JR, Succar J, Xin X, Wang X. Transversus abdominis-plane block versus local anesthetic wound infiltration in lower abdominal surgery: a systematic review and metaanalysis of randomized controlled trials. BMC Anesthesiol 2014; 14: 121. DOI: https://doi.org/10.1186/1471-2253-14-121
Jin Y, Li Y, Zhu S, Zhu G, Yu M. Comparison of ultrasound-guided iliohypogastric/ilioinguinal nerve block and transversus abdominis plane block for analgesia after cesarean section: A retrospective propensity match study. Exp Ther Med 2019; 18: 289-95 DOI: https://doi.org/10.3892/etm.2019.7540
Downloads
Published
How to Cite
Issue
Section
License
The Journal of Southeast Asian Medical Research will hold the copyright to all published articles. The publisher's production department handles copyright forms once a manuscript is accepted and scheduled for publication.







